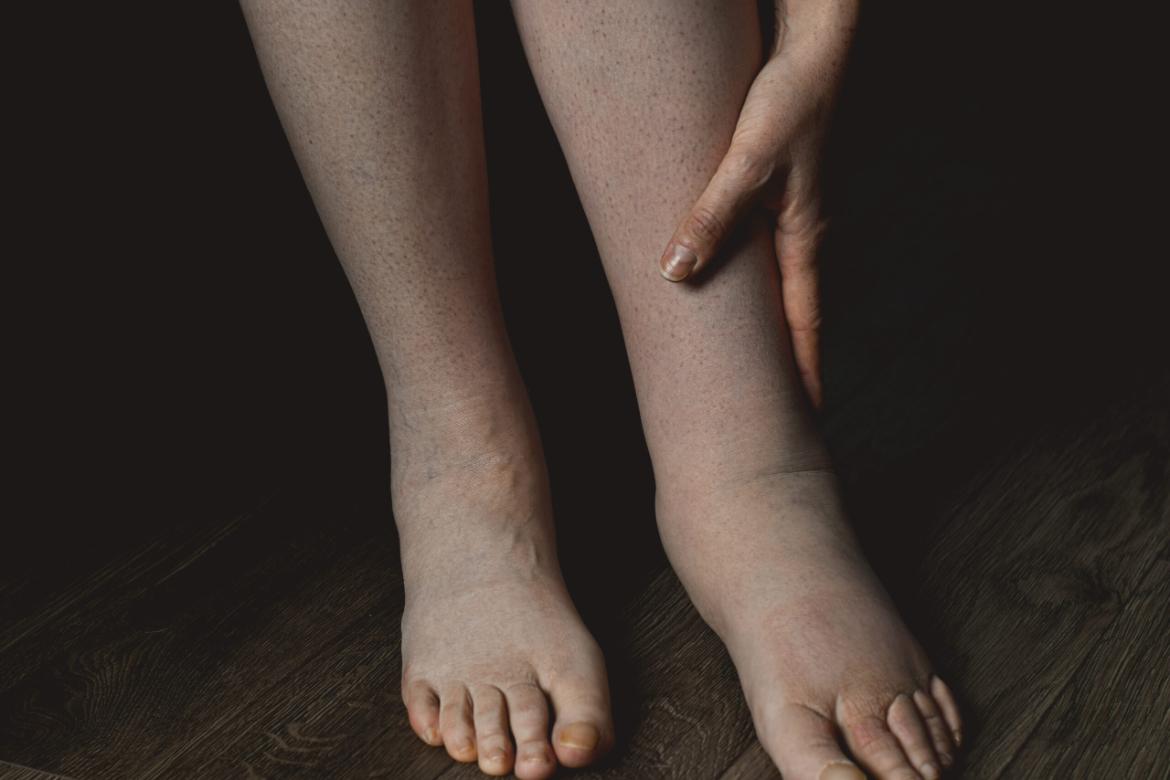
Lymphedema (Elephantiasis)
Lymphedema is a condition in which lymph fluid accumulates due to a blockage or damage to the lymphatic system. The lymphatic system is a circulatory system that works in conjunction with the body's immune system. Lymph fluid collects waste products and excess fluid from the tissues and transports them to the lymph nodes. Lymph nodes are the sites where lymphocytes, the body's defense mechanism, are produced and stored.
Lymphedema typically manifests as swelling and a feeling of heaviness in the arms or legs. This condition occurs when lymph fluid doesn't circulate normally. It can be caused by a variety of factors, including blockage or damage to the lymphatic system, weakened lymph vessels, or removal of lymph nodes.
What are the symptoms of lymphedema?
Lymphedema, or elephantiasis, is a condition in which lymph fluid accumulates due to a blockage or damage to the lymphatic system. This condition typically manifests as swelling and a feeling of heaviness in the arms or legs. Some symptoms of lymphedema include:
- Arm or leg swelling: Lymphedema is characterized by swelling, usually in one or both arms or legs. This swelling can increase and become firm over time. The swelling often begins in the hand or foot and progresses upward. It can be particularly noticeable in joint areas such as the ankles, wrists, fingers, or toes.
- A feeling of heaviness and fullness: A feeling of heaviness and fullness in the lymphedema area is a common symptom. This feeling is usually caused by swelling.
- Skin thickening and hardening: The skin in the area of lymphedema may thicken and harden. The skin's texture may change and take on a lumpy or rough appearance.
- A feeling of tightness and squeezing: The skin in the lymphedema area may become tight and feel tight. This can occur as swelling increases.
- Pain and tenderness: Pain and tenderness may be experienced in the lymphedema area. Pain may increase, especially with touch or pressure.
- Limited mobility: Lymphedema can affect joint mobility and cause limited movement. Swelling and stiffness can make it difficult to move an arm or leg normally.
- Increased risk of infection: The accumulation of lymph fluid and the disruption of lymphatic drainage increase the risk of infection. Frequent infections, especially bacterial infections called cellulitis, can occur in areas with lymphedema.
Lymphedema symptoms can vary from person to person and depend on the stage of disease progression. If you experience any of the symptoms of lymphedema, it's important to seek medical attention.
What are the causes of lymphedema?
Lymphedema, or elephantiasis, occurs when lymph fluid accumulates, usually due to a blockage or damage to the lymphatic system. This blockage or damage prevents the normal circulation of lymph fluid, causing swelling. Lymphedema can often develop due to:
- Surgical procedures: Surgery that affects the lymphatic system can increase the risk of lymphedema. Lymphedema can develop as a result of lymph node removal or damage to the lymphatic system, particularly during cancer treatment.
- Radiation therapy: Radiation used for cancer treatment can increase the risk of lymphedema. Radiation can damage the lymphatic system and interfere with the normal circulation of lymph fluid.
- Genetic factors: Some cases of lymphedema can be passed down genetically. Congenital disorders or a family history may increase the risk of lymphedema.
- Infections: A serious infection can contribute to the development of lymphedema by damaging the lymphatic system. Infections that damage the lymph nodes or lymph vessels, in particular, can lead to lymphedema.
- Trauma or injuries: Trauma or injuries to the lymphatic system can block the normal flow of lymph fluid and lead to lymphedema.
- Liver cirrhosis: Some liver diseases, such as liver cirrhosis, can cause lymph fluid to accumulate in the body and trigger the development of lymphedema.
- Obesity : Obesity can affect the circulation of lymph fluid and increase the risk of lymphedema.
Lymphedema often occurs due to a combination of these causes. In any case, any factor that interferes with the normal circulation of lymph fluid can contribute to the development of lymphedema. Patients with lymphedema should work with a healthcare professional to minimize risk factors and manage symptoms.
What are the types of lymphedema?
- Primary Lymphedema: Primary lymphedema is a congenital or genetically transmitted condition. It develops due to congenital abnormalities or gene mutations in the lymphatic system. Primary lymphedema is generally classified into three subtypes:
- Congenital Lymphedema (Milroy Disease): This type of lymphedema can be seen from birth. Lymph fluid accumulates because the lymph vessels are congenitally missing or abnormal.
- Meige's lymphedema (Meige's disease): Meige's lymphedema, which usually occurs in adolescence or adulthood, is caused by the abnormal development of lymphatic vessels or the absence of certain lymphatic vessels, leading to an accumulation of lymph fluid.
- Lymphedema Praecox: Lymphedema praecox usually begins in adolescence or young adulthood. It's a developmental abnormality in the lymphatic system that causes lymph fluid to accumulate.
- Secondary Lymphedema: Secondary lymphedema is a condition that develops due to another cause. Obstruction or damage to the lymphatic system causes lymph fluid to accumulate. Secondary lymphedema can often occur in the following situations:
- Surgical interventions: The flow of lymph fluid may be blocked as a result of removal of lymph nodes or surgical interventions in the lymphatic system.
- Radiation therapy: Radiation used for cancer treatment can damage the lymphatic system, causing lymphedema.
- Infections: Infections that damage the lymph nodes or lymph vessels can contribute to the accumulation of lymph fluid and the development of lymphedema.
- Cancer: Cancer can cause blockage or damage to the lymphatic system and contribute to lymphedema.
How is lymphedema diagnosed?
Lymphedema is usually diagnosed through a clinical examination and symptom assessment. Below are common methods and diagnostic steps used to diagnose lymphedema:
- Hospital History and Physical Examination: The doctor will review the patient's medical history and symptoms. The patient's narrative will be listened to to learn about the presence of lymphedema symptoms, their duration, severity, and progression. During the physical examination, swelling, skin changes, tissue hardness, and other symptoms will be examined.
- Lymphedema Measurements: The circumference of the lymphedema area is measured to assess the level of swelling. These measurements are used to monitor swelling in the lymphedema area and assess response to treatment.
- Lymphedema Analysis: Lymphedema analysis is rarely used to diagnose lymphedema. This method involves sending a sample from the affected area for laboratory analysis. Lymphedema diagnosis can be supported by evaluating the protein level and other parameters in the lymphedema.
- Imaging Tests: Imaging tests may be used to confirm a diagnosis of lymphedema and to identify damage to the lymphatic system. These may include lymphograms (X-rays made with the injection of contrast material), lymphedema magnetic resonance imaging (MRI), and lymphedema computed tomography (CT).
Diagnosing lymphedema may require a multidisciplinary approach. It is typically performed by a lymphedema specialist or a healthcare team experienced in lymphedema treatment. Other possible conditions (e.g., venous edema) must be excluded during the diagnostic process.
Lymphedema is diagnosed by combining symptoms, physical examination findings, and other test results. Making the correct diagnosis is crucial for developing an appropriate treatment plan and initiating lymphedema management.
How is lymphedema treated?
Treatment for lymphedema aims to improve lymphatic circulation and reduce swelling. Treatment typically requires a multidisciplinary approach and may include the following:
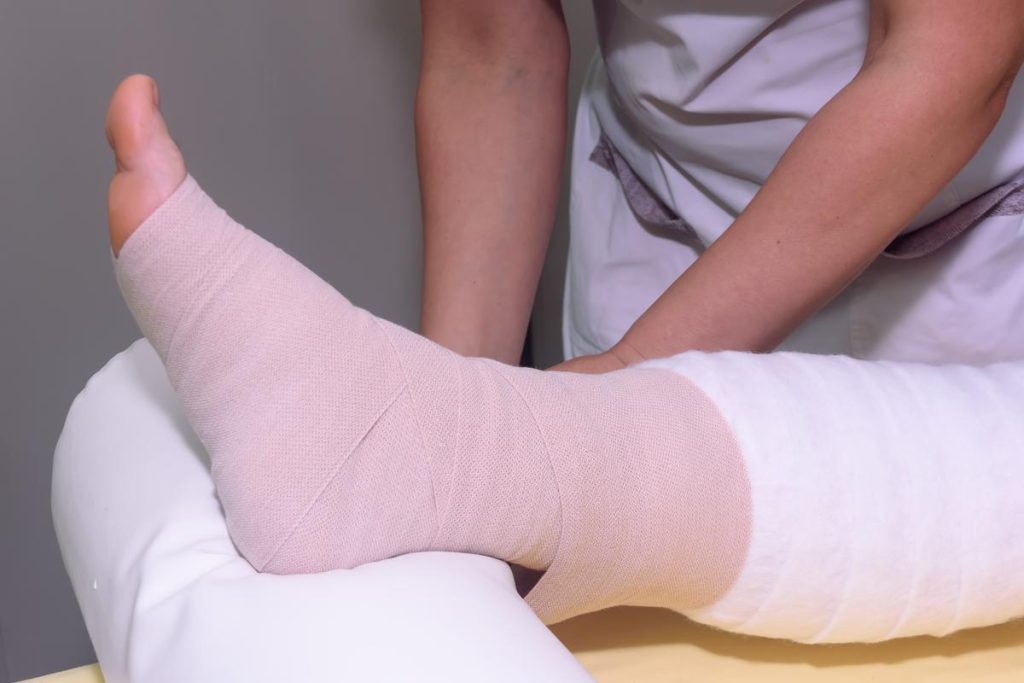
- Compression Therapy: Compression therapy is a method used to reduce swelling in areas where lymph fluid accumulates. This involves the use of pressure bandages or compression garments (e.g., compression arm bandages, compression stockings). Compression promotes the movement of lymph fluid and increases lymphatic flow.
- Lymphatic Drainage Therapy (LDT): Lymphatic drainage therapy is a massage technique used to increase lymphatic circulation and direct accumulated lymph fluid. It is administered by a qualified physical therapist or licensed lymphedema therapist. This therapy helps reduce swelling in the affected area.
- Exercise: Regular exercise is important to increase lymphatic circulation and support the muscle pump effect. Specific exercises recommended by a qualified physical therapist can help manage lymphedema.
- Skin Care : The skin in areas with lymphedema may be sensitive and at increased risk of infection. Proper skin care helps reduce the risk of infection. This includes cleansing, moisturizing, preventative measures (e.g., avoiding injury), and hygienic practices.
- Weight Management: Obesity can worsen lymphedema symptoms. Maintaining a healthy weight or losing weight can help manage lymphedema.
- Surgical Interventions: In rare cases, surgical options may be considered for the treatment of lymphedema. Surgical interventions may be performed to improve lymphatic flow or to repair swollen tissue and damaged lymphatic structures.
The treatment plan is personalized based on the patient's symptoms, the type of lymphedema, the progression of the disease, and their overall health. Treatment focuses on managing the lymphedema and controlling symptoms.

