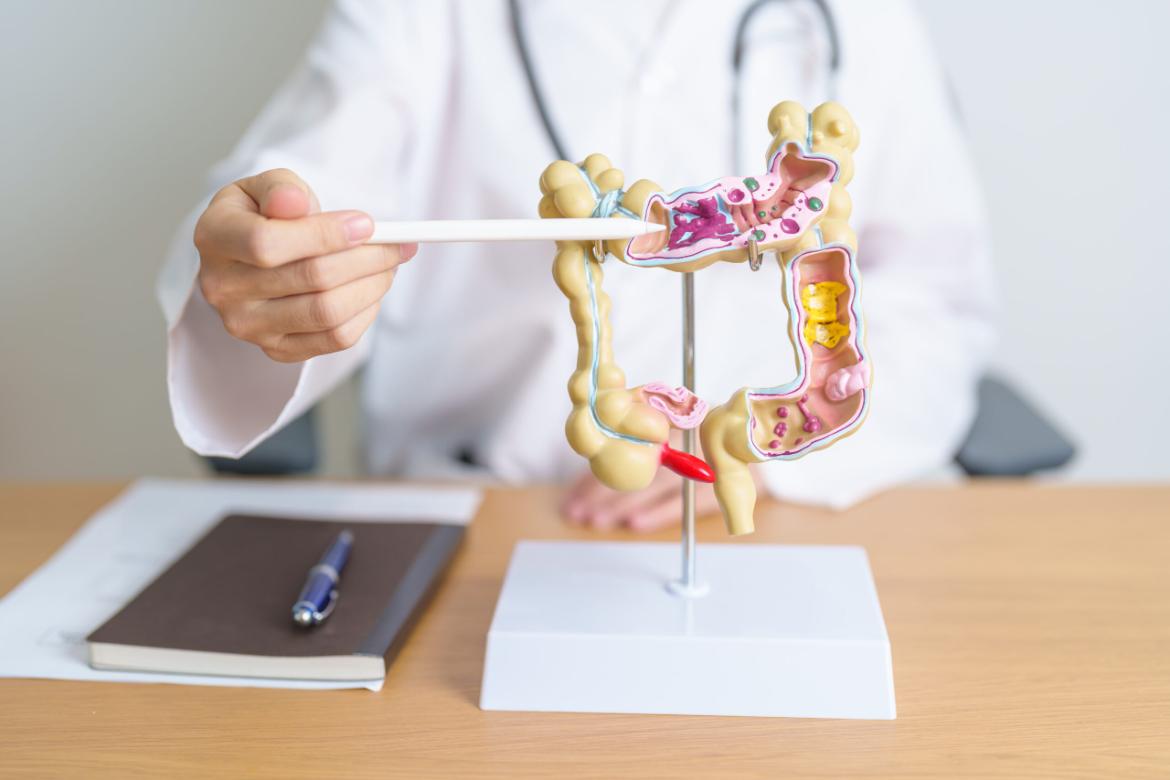
Diverticulitis
Diverticulitis is the inflammation of pouches called diverticula, located in the lining of the colon. Diverticula are small pouches that usually form in the large intestine and are caused by weakened intestinal walls. Diverticulitis occurs when stool accumulates within these pouches, causing inflammation or infection.
Diverticulitis is most common in older adults and is usually an advanced stage of diverticular disease. This disease typically results from infection of diverticula in the colon by microorganisms.
Diverticulitis Symptoms
Diverticulitis symptoms can vary depending on the severity of the disease and the extent of inflammation. Some people experience mild symptoms, while others may have more severe symptoms. Diverticulitis symptoms may include:
- Abdominal pain: The most common symptom of diverticulitis is abdominal pain. It usually occurs in the lower left abdomen. The pain usually begins suddenly and can be severe. In some people, the pain may worsen with movement or going to the bathroom.
- Fever: Diverticulitis is often associated with inflammation, which can cause an increase in body temperature. Patients may experience a fever.
- Constipation or diarrhea: Diverticulitis can sometimes affect bowel movements. This can result in either constipation or diarrhea. In some patients, both conditions can occur simultaneously.
- Gas and bloating: Intestinal problems caused by diverticulitis can lead to gas accumulation and bloating.
- Nausea and vomiting : If diverticulitis is severe, gastrointestinal symptoms such as nausea and vomiting may occur.
- Loss of appetite: Patients may report a loss of appetite due to diverticulitis.
- Bloody stools : In some cases, the inflammation caused by diverticulitis can cause blood to appear in the stool. The blood is usually bright red or dark red on the stool.
Diverticulitis symptoms can vary from person to person and can sometimes be confused with symptoms of other health problems. If you suspect you have diverticulitis, it's important to consult a healthcare professional.
Causes of Diverticulitis
Diverticulitis is a condition that results from inflammation of diverticula in the large intestine. Diverticula are small pouches that form as a result of weakening of the intestinal wall. The primary cause of diverticulitis is inflammation or infection from stool accumulating within these pouches. However, some factors that contribute to the development of diverticulitis include:
- Stool buildup: Stool buildup inside diverticula increases the risk of inflammation and infection. If this buildup causes blockage or pressure in the diverticula, inflammation can develop.
- Dietary habits: A low-fiber diet can lead to constipation and slow bowel movements. A lack of fiber can cause stools to become soft and accumulate more easily in the colon, increasing the risk of inflamed diverticula.
- Aging : Diverticular disease generally increases with age. The aging process can reduce the elasticity of the intestinal wall, making it more likely that diverticula will form.
- Genetic factors: Individuals with a family history of diverticular disease may have a slightly higher risk of developing the disease. Genetic predisposition is thought to play a role in the development of diverticulitis.
- Smoking: Smoking can negatively impact gut health and contribute to weakening of the bowel wall, accumulation of stool, and an increased risk of inflamed diverticula.
- Obesity : Obesity can affect bowel movements and increase the risk of developing diverticular disease.
- Intestinal motor dysfunction : If the intestinal muscles do not function properly, this can cause stool to accumulate inside the diverticula, increasing the risk of inflammation.
Although the causes of diverticulitis are still not fully understood, the factors mentioned above are thought to play a role in the formation of diverticulitis.
Who is at Risk for Diverticular Disease?
Diverticular disease is a condition in which pouches called diverticula form in the colon. However, the risks associated with inflammation of diverticular disease, such as diverticulitis, become more significant. Some factors and risk groups associated with the development of diverticular disease include:
- Age: Diverticular disease generally increases with age. It is particularly common after age 40.
- Lack of fiber: A diet low in fiber can make bowel movements difficult and cause constipation, which can contribute to the development of diverticular disease.
- Low physical activity: A sedentary lifestyle can slow bowel movements and contribute to the development of diverticular disease.
- Obesity : Obesity may increase the risk of diverticular disease.
- Smoking : Smoking can negatively impact bowel health and increase the risk of diverticular disease.
- Family history: People with a family history of diverticular disease may have a slightly higher risk of developing the disease.
- Inflammation: Those who have previously had inflammation due to diverticular disease are at risk of developing diverticulitis.
- Intestinal motor dysfunction: In some people, problems with bowel movements and weakness of the intestinal muscles may play a role in the development of diverticular disease.
These factors and risk groups are considered general risk factors for diverticular disease. However, anyone can be at risk for developing diverticular disease. If you are concerned about your symptoms or risk factors for diverticular disease, it is recommended that you consult a healthcare professional. They can provide you with more information about appropriate diagnosis and treatment options.
What are the ways to prevent diverticulitis?
- A high-fiber diet: A high-fiber diet softens stools and regulates bowel movements. This helps reduce stool accumulation in diverticula and lowers the risk of inflammation. Consuming vegetables, fruits, whole grains, legumes, and adequate water are key elements of a high-fiber diet.
- Hydration: Drinking enough water helps soften stools and regulate bowel movements. It's important to consume enough water daily.
- Physical activity: Regular physical activity increases bowel movements and prevents constipation. Incorporating walking, running, exercise, or any other activity into your daily routine can be beneficial.
- Quit smoking: Smoking can negatively impact gut health and increase the risk of diverticulitis. Quitting smoking can help promote a healthier gut and reduce the risk of inflammation.
- Regular toileting habits: Continuously postponing the need to go to the toilet can cause stool to accumulate in the intestines, increasing the risk of inflamed diverticula. It's important to go to the toilet on time when you need to.
- Stress management: Stress can affect bowel movements and increase the risk of diverticulitis. Stress management techniques can help maintain gut health by reducing your stress levels.
- Regular medical checkups: It's especially important to schedule regular checkups with your doctor if you have diverticular disease. This way, you can monitor your health and take preventative measures if necessary.
While diverticulitis cannot be completely prevented, following the methods above can help reduce your risk of developing it. If you experience symptoms of diverticulitis or have risk factors, it's important to consult a healthcare professional for information about appropriate treatment and prevention strategies.
Diverticulitis Diagnosis
Physical exam: The doctor will perform a physical exam to assess the patient's signs and symptoms. This includes checking for signs such as tenderness, swelling, or pain in the abdominal area.
Blood tests: Blood tests may be used to assess markers of inflammation (such as white blood cells and C-reactive protein). These tests can help determine the presence and severity of inflammation.
Radiologic imaging: Radiologic imaging plays an important role in diverticulitis diagnosis. These may include:
- Computed tomography (CT) scan: A CT scan is used to visualize diverticula and inflammation. This provides a detailed examination to rule out other bowel diseases.
- Colonoscopy : A colonoscopy is a procedure used to examine the lining of the intestine. A flexible tube called an endoscope is inserted through the anus into the intestine, allowing the doctor to assess the presence of diverticula and inflammation in the intestinal wall. A sample may also be taken for biopsy.
Other imaging methods: In some cases, other imaging methods such as ultrasound or magnetic resonance imaging (MRI) may also be used.
Diagnosis of diverticulitis begins with a physical examination based on the patient's signs and symptoms, and is then confirmed with imaging studies. To make a diagnosis, your doctor will recommend appropriate tests and imaging studies.
Diverticulitis Treatment
Treatment for diverticulitis can vary depending on the severity of symptoms, the presence of complications, and the patient's overall health. Treatment typically involves:
- Antibiotic therapy: In cases of mild or moderate inflammation from diverticulitis, doctors usually prescribe oral antibiotics. Antibiotics are used to control inflammation and treat infection.
- Fluid and diet changes: During the acute phase of diverticulitis, a liquid diet can be implemented to rest the intestines. This reduces pressure on the intestines and promotes healing. Later, a fiber-rich diet can be gradually introduced. Fiber softens stools and regulates bowel movements. Your doctor will determine the appropriate diet for you.
- Pain relievers and anti-inflammatory medications: Pain relievers and anti-inflammatory medications may be prescribed to control pain and inflammation. However, it's important to consult your doctor before using these medications.
- Hospitalization: In cases where diverticulitis causes serious complications or other health problems, hospitalization may be necessary. Hospitalization may include intravenous antibiotics and fluids. In addition, in some cases, surgery may be necessary.
- Surgery: Surgery may be considered when diverticulitis causes serious complications or recurrences. Surgical removal of the diverticula (colectomy) or removal of a portion of the intestine may be necessary. However, surgery is only performed in certain circumstances and under the guidance of your doctor.
Diverticulitis treatment is customized to each patient's condition. The goals are to relieve symptoms, control inflammation, treat infection, and prevent complications. It's important to follow your doctor's recommendations and schedule regular checkups throughout the treatment process.
What Should Diverticulosis Patients Avoid?
Some people with diverticular disease may find that certain foods can worsen symptoms. However, because each patient is different, it's difficult to say which specific foods are right for everyone. However, the following foods may be potentially problematic for some people with diverticulitis:
- Low-fiber foods: A lack of fiber can worsen symptoms of diverticular disease. Therefore, it's recommended to avoid low-fiber foods like white bread, white rice, processed grains, and sugary snacks.
- Small seeds : Some people believe that small seeds can become lodged in diverticula and cause discomfort in patients with diverticular disease. Therefore, limiting or avoiding foods with small seeds, such as grape seeds, strawberry seeds, tomato seeds, and sesame seeds, may be recommended.
- Nuts: Nuts may contain potential irritants that can trigger diverticulitis symptoms. Therefore, limiting or avoiding nuts such as walnuts, almonds, hazelnuts, and peanuts may help some people.
- Spicy and hot foods : Spicy and hot foods can cause intestinal irritation and exacerbate diverticulitis symptoms in some people. Therefore, avoiding or limiting consumption of these foods, such as hot peppers, spicy sauces, and spices, may be recommended.
If you find that any of the above foods worsen your symptoms, it's important to adjust your diet based on your individual tolerance. However, it's important for anyone with diverticular disease to tailor their diet to their individual needs and consult with a nutritionist or doctor. This way, you can assess whether certain foods are appropriate for you and create a healthy diet plan.

