Inflammatory Bowel Disease
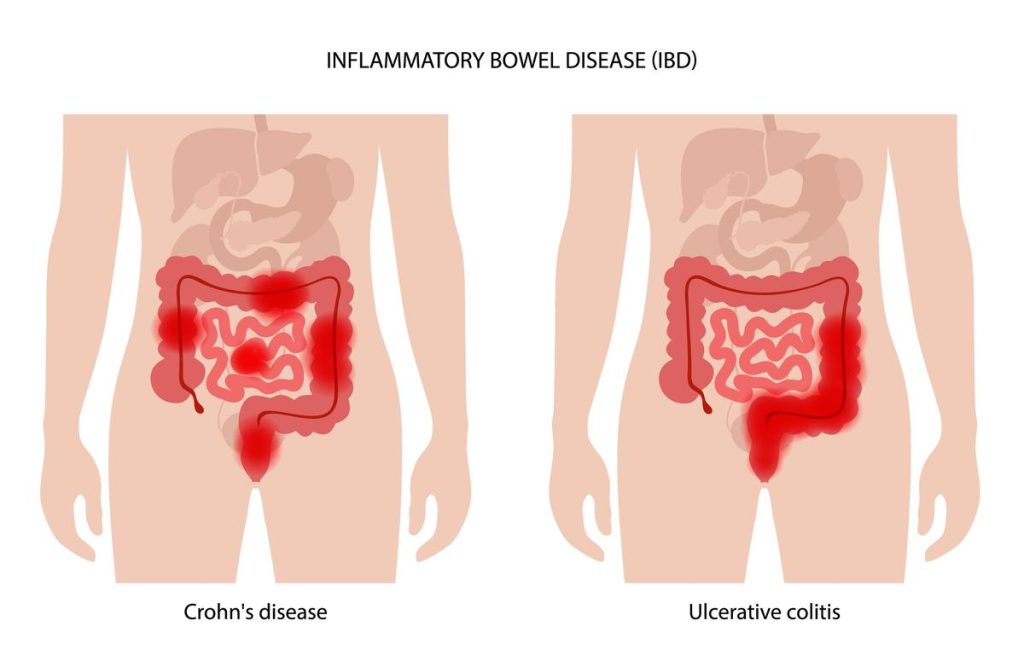
Inflammatory bowel disease (IBD) is a general term that describes a range of diseases characterized by chronic inflammation of the intestines. IBD includes two main types: Crohn's disease and ulcerative colitis. These diseases cause long-term, recurring inflammation of the intestines and can affect different areas throughout the digestive tract.
- Crohn's disease: Crohn's disease is a chronic inflammatory disease that can affect any part of the digestive system and involves all layers of the intestinal wall. It most commonly affects the lower part of the small intestine (the ileum) and the large intestine, but can occur in any part of the digestive system. Healthy bowel segments are often located between the inflamed areas, hence the name "skip lesions." Crohn's disease can lead to sores, ulcers, and strictures in the intestines.
- Ulcerative colitis: Ulcerative colitis is an inflammatory disease that affects only the large intestine (colon and rectum). It typically begins in the rectum and spreads continuously throughout the large intestine. The disease causes ulcers to form in the intestinal wall, which can lead to symptoms such as bleeding, diarrhea, and abdominal pain.
Inflammatory bowel disease causes
Although the causes of inflammatory bowel disease (IBD) are not fully understood, several factors are thought to contribute to its development. The primary cause of IBD is an excessive and abnormal immune system response against the normal intestinal flora. This process causes inflammation, ulcers, and sores in the intestinal wall. Some factors that contribute to the development of IBD include:
- Genetic predisposition: People with a family history of IBD are more likely to develop the disease. Genetic factors play a significant role in the development of inflammatory bowel disease. Certain genetic mutations, particularly for Crohn's disease, have been identified.
- Immune system irregularities: One of the main causes of IBD is an incorrect immune response to the intestines. Normally, the immune system is designed to protect the body from infection. However, in people with IBD, the immune system overreacts to harmless microbes in the intestines, leading to inflammation.
- Environmental factors : Environmental factors may play a role in the development of IBD. Environmental factors such as smoking, environmental pollution, and the consumption of certain foods are thought to be influential in the development of the disease.
- Gut flora imbalance: Hundreds of different species of bacteria live in our intestines, and these bacteria significantly impact our immune system, digestion, and intestinal health. In IBD, imbalances in the gut flora can contribute to the development of the disease.
- Immune system viruses : It is thought that some viruses may cause the immune system to target the intestines, leading to inflammation.
Pinpointing the causes of IBD and finding a definitive solution is challenging. However, in individuals with a genetic predisposition, avoiding environmental factors and making lifestyle changes can help reduce the risk of developing the disease. Early diagnosis and effective treatment can help control IBD symptoms and improve patients' quality of life.
Inflammatory bowel disease symptoms
The symptoms of inflammatory bowel disease (IBD) can vary depending on the type and severity of the disease. The two main types of IBD, Crohn's disease and ulcerative colitis, can cause similar symptoms, but some differences can also occur. Common symptoms of IBD include:
- Abdominal pain and cramps: Cramp-like pain in the abdominal area, especially in the lower abdomen or right lower quadrant, are common symptoms.
- Diarrhea: Loose or frequent bowel movements, sometimes accompanied by bloody or slimy stools.
- Bloody stools: Blood may be seen in the stool, especially in diseases such as ulcerative colitis.
- Loss of appetite and weight loss : Inflammation of the intestines can affect nutrient absorption, which can lead to loss of appetite and weight loss.
- Fatigue and weakness: Chronic inflammation and loss of stool can lead to lack of energy and fatigue in the body.
- Nausea and vomiting: Nausea and vomiting may occur due to intestinal obstruction, especially in Crohn's disease.
- Fever: During IBD attacks, body temperature may tend to rise.
- Joint pain : In some cases of IBD, joint pain and swelling may occur.
- Eye and skin problems: IBD can cause problems such as redness, pain, or inflammation of the eyes and skin rashes and ulcers.
These symptoms may vary depending on the severity of IBD, the area of the intestine affected, and the stage of the disease.
Diagnostic methods for inflammatory bowel diseases
- Medical history and physical examination : The first step is to assess the patient's symptoms and health history. The gastroenterologist will examine the patient's abdomen and look for typical signs of IBD.
- Blood tests: Blood tests are done to evaluate signs of inflammation and other biochemical changes in the body. For example, tests such as CRP (C-reactive protein) and sedimentation rate can indicate inflammation in the body.
- Stool tests: Analysis of a stool sample can help identify blood, infection, and other intestinal problems. It can also look for occult blood or markers of inflammation in the stool.
- Endoscopy : Endoscopy is a method of visually examining the inside of the digestive system using a thin tube (endoscope) equipped with a camera. Endoscopy plays a particularly important role in the diagnosis of ulcerative colitis and Crohn's disease. Endoscopic procedures such as colonoscopy (for the large intestine) and gastroscopy (for the stomach) may be used.
- Colon biopsy: Tissue samples (biopsies) taken during endoscopy are examined under a microscope to evaluate inflammation, ulcers, and other lesions in the bowel wall.
- Radiologic imaging: Imaging techniques such as computed tomography (CT) scans and magnetic resonance imaging (MRI) can provide detailed images of the intestines and other digestive organs. These images can help determine the extent of disease and the affected areas.
These diagnostic methods help establish a definitive diagnosis of IBD. Depending on the type of IBD and the severity of the disease, multiple tests and evaluations may sometimes be necessary to establish a diagnosis. Early diagnosis, appropriate treatment, and follow-up can help control symptoms and improve the patient's quality of life.
Inflammatory bowel disease treatment
Treatment for inflammatory bowel disease (IBD) is personalized based on the type and severity of the disease, the affected areas, and the patient's overall health. Treatment focuses on reducing symptoms, controlling inflammation, preventing relapses, and preventing complications. The following methods and medications may be used in the treatment of IBD:
Drug therapy:
- Anti-inflammatory medications: Anti-inflammatory medications such as steroids and aminosalicylates are used to reduce inflammation in the intestinal wall.
- Immunosuppressants: When the immune system is overactive in IBD, immunosuppressant medications may be used. These can help control inflammation and prevent relapses.
- Biological agents: Biological agents called monoclonal antibodies can help control the inflammatory process by targeting immune system cells. d. Antibiotics: May be used if there is an infection in the intestine or to prevent complications.
Nutrition and diet changes:
- During periods of BD, it has been observed that certain foods can exacerbate symptoms. Individuals may try to alleviate symptoms by avoiding certain foods, depending on their individual tolerance.
- Nutritionists can provide support to patients regarding food allergies or intolerances and help patients maintain adequate nutritional levels.
Surgical Treatment:
- In severe cases of IBD, surgery may be necessary. This surgery may be performed to correct intestinal narrowing or obstructions, treat fistulas or abscesses, or remove damaged sections of intestine.
Lifestyle Changes:
- Stress management: Stress can exacerbate IBD symptoms. Methods such as meditation, yoga, or exercise can be used to reduce stress.
- Quitting smoking: Smoking can worsen IBD symptoms. IBD patients may benefit from controlling their symptoms by quitting smoking.
Treatment can alter the course of IBD, achieving periods of remission and reducing symptoms. However, due to the chronic nature of the disease, ongoing monitoring and management may be necessary. It is important for IBD patients to collaborate with a gastroenterologist or registered dietitian throughout the treatment process. This allows them to determine the most appropriate treatment plan and lifestyle changes, improving their quality of life.
How can inflammatory bowel diseases be prevented?
Because the exact causes of inflammatory bowel disease (IBD) are not fully understood, it can be difficult to completely prevent the disease. However, certain preventive measures and lifestyle changes can help reduce the risk of IBD or manage its symptoms. Here are some steps you can take to help prevent IBD:
- Healthy diet: A balanced and healthy diet can help maintain intestinal health. High-fiber foods, fresh fruits and vegetables, whole grains, and foods containing probiotics can help maintain a healthy intestinal flora.
- Smoking and alcohol: Smoking and excessive alcohol consumption can increase the risk of IBD and worsen symptoms. Quitting smoking and limiting alcohol are important steps to maintain gut health.
- Stress management: Stress can trigger or exacerbate IBD symptoms. Practicing relaxation techniques such as meditation, yoga, exercising, and engaging in hobbies can be helpful to manage stress.
- Avoiding infections: Some infections can contribute to intestinal inflammation. Practicing good hygiene and maintaining good handwashing habits can help reduce the risk of infection.
- Family history: If IBD runs in your family, it's important to have regular medical checkups and catch symptoms early to reduce your risk.
- Medication use: For people with IBD symptoms, following medication regularly as recommended by their doctor can help control symptoms and prevent relapses.
It's important to remember that IBD is sometimes not preventable because its causes are not fully understood. However, the measures above can help reduce the risk or manage the disease. If you suspect you have any symptoms or risk factors for IBD, it's important to consult a gastroenterologist for an evaluation and take appropriate preventative measures. Early diagnosis and appropriate treatment can prevent the progression of IBD and improve quality of life.
What are the complications of inflammatory bowel disease?
Inflammatory bowel disease (IBD) is a chronic inflammatory bowel disease with two main types: Crohn's disease and ulcerative colitis. IBD causes long-term, recurring inflammation in the intestines and can lead to various complications over time. Some of the common complications of IBD include:
- Intestinal obstruction
- Intestinal perforation
- Abdominal abscesses
- Fistulas
- Internal bleeding
- Anemia
- Joint problems
- Skin problems
- Liver problems
- Eye problems
- Loss of bone density
Good management of IBD symptoms, medication, dietary and lifestyle changes, surgical interventions, and regular follow-up can help prevent or alleviate these complications.
Can inflammatory bowel diseases cause cancer?
Yes, inflammatory bowel disease (IBD) can increase the risk of developing colon cancer due to long-term, chronic inflammation. The two main types of IBD, Crohn's disease and ulcerative colitis, cause persistent inflammation in the intestines, which can increase the likelihood of developing cancer over time.
The main reason IBD increases cancer risk is that chronic inflammation leads to cell damage and mutations. Mutations can cause normal cells to mutate into cancer cells, leading to cancer development.
Colorectal cancer (colon cancer and rectal cancer) are among the cancers associated with IBD. Therefore, individuals diagnosed with IBD, especially those with long-standing and widespread inflammation, should be regularly monitored and undergo cancer screening tests. Early diagnosis can increase the chances of colorectal cancer treatment and preventative measures.
Remember, cancer risk can be different for each patient, and it is important to talk to your doctor about your individual situation.

