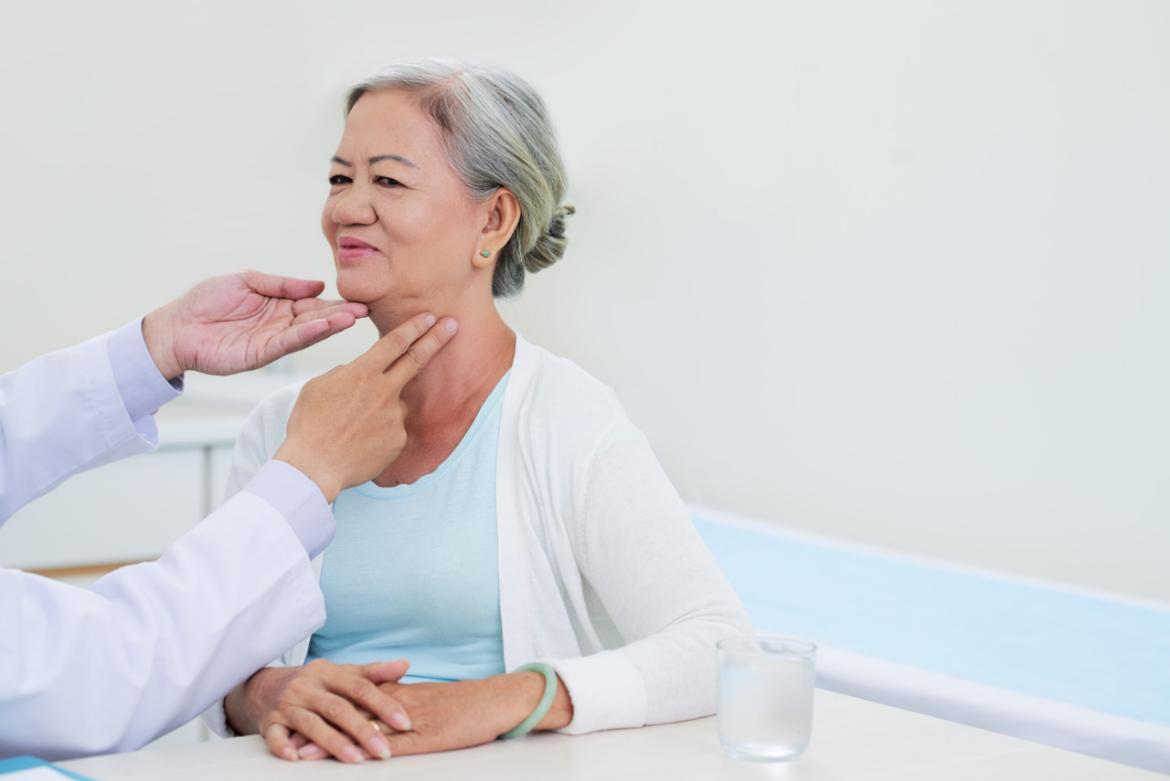
Adenitis
Adenitis refers to inflammation of the lymph nodes. As part of the immune system, lymph nodes produce infection-fighting cells and filter out harmful microorganisms. Adenitis occurs when these glands become infected or inflamed.
Types of Adenitis?
The types of adenitis can vary depending on the underlying cause of the inflamed lymph nodes. Common types include:
- Bacterial adenitis: This occurs as a result of bacterial infections. For example, bacterial infections such as streptococcal throat, staphylococcal skin infections, tuberculosis, or brucellosis can cause inflammation of the lymph nodes.
- Viral adenitis: Develops as a result of viral infections. Viral infections such as the common cold, flu, Epstein-Barr virus (mononucleosis), or HIV can cause inflammation of the lymph nodes.
- Lymphoma-associated adenitis: Lymphoma is cancer of the lymphatic system. It is characterized by the accumulation of abnormal cells in the lymph nodes. Lymphoma can cause the lymph nodes to become swollen and inflamed.
- Nonspecific adenitis: Inflammation of the lymph nodes due to non-infectious causes. These may include trauma, irritation, allergic reactions, or immune system diseases.
- Tuberculous adenitis: Tuberculosis, an infection caused by tuberculosis bacteria, can cause inflammation of the lymph nodes. Tuberculous adenitis usually occurs in groups of lymph nodes, such as those in the neck or armpit.
These are just some examples, there may be more variations.
What are the causes of adenitis?
Inflammation of the lymph nodes can be caused by a variety of factors. Common causes include:
- Bacterial infections : One of the most common causes is bacterial infections. Bacterial infections such as streptococcal throat infections, staphylococcal skin infections, tuberculosis, brucellosis, and skin wounds can cause inflammation in the lymph nodes.
- Viral infections: Viruses can also cause adenitis. Viral infections such as the common cold, the flu, Epstein-Barr virus (mononucleosis), cytomegalovirus (CMV), and HIV can cause inflammation of the lymph nodes.
- Oral or dental infections: Oral and dental infections such as gum infections, tooth abscesses, or cavities can cause inflammation of the lymph nodes in the neck.
- Immune system disorders: Immune system disorders can cause inflammation of the lymph nodes. For example, autoimmune diseases such as lymphocytic hyperplasia, where lymphocytes are overproduced, or rheumatoid arthritis can cause adenitis.
- Cancer: Some cancers, especially cancers of the lymphatic system such as lymphoma or leukemia, can lead to inflammation of the lymph nodes.
- Immunosuppressive therapy: Treatments that suppress the immune system can cause inflammation of the lymph nodes after organ transplants or when using immunosuppressive drugs.
- Other causes: Adenitis can sometimes be due to nonspecific factors whose cause is not clearly identifiable. These factors may include trauma, irritation, allergic reactions, or inflammatory diseases.
For a complete diagnosis of the cause, it's important to see a doctor who will evaluate your symptoms and medical history. Treatment varies depending on the underlying cause and may include controlling the infection or other appropriate treatments.
What are the symptoms of adenitis?
- Swollen lymph nodes: The most obvious symptom is enlargement and swelling of the inflamed lymph node. The swollen lymph node is often painful and tender.
- Pain and tenderness: Inflamed lymph nodes can be painful and become more tender under pressure.
- Redness and warmth: Redness and a slight warmth may be observed in the lymph node area affected by adenitis.
- General symptoms: Because adenitis is often the result of an infection, symptoms related to the infection may also be observed. These may include fever, fatigue, headache, muscle aches, sore throat, runny nose, cough, diarrhea, or vomiting.
- Local symptoms: Depending on the source of the infection, specific symptoms may also appear at the site of infection. For example, adenitis caused by a throat infection may cause a sore throat and a red throat. Adenitis caused by a toothache may also cause symptoms of tooth decay.
Symptoms can vary depending on the type of disease, the extent of infection, and the individual's immune system response.
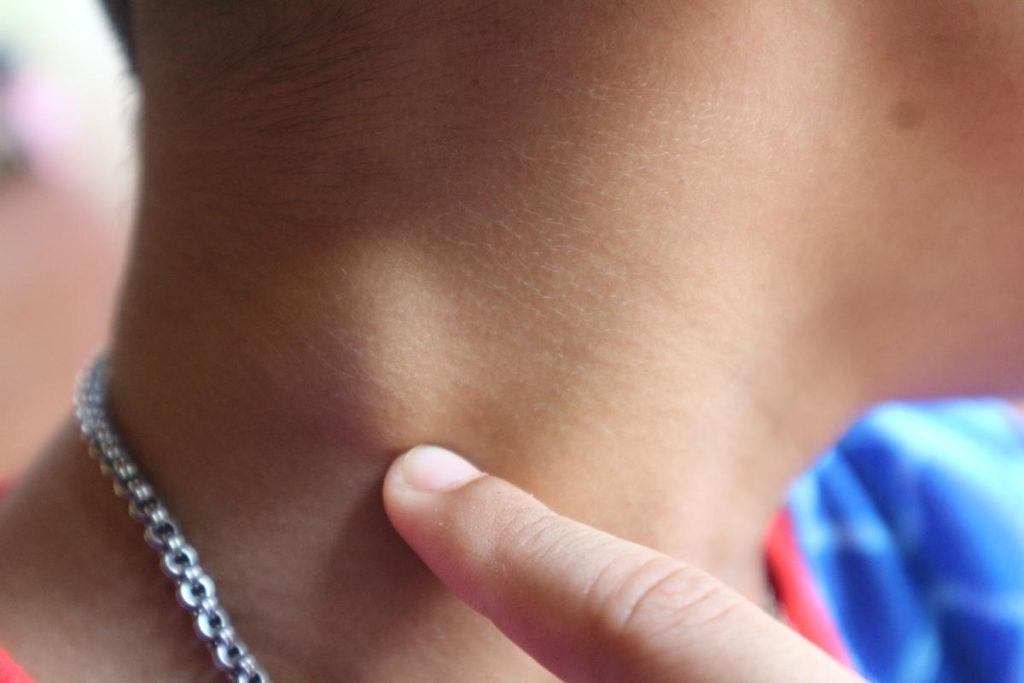
How is Adenitis Diagnosed?
Adenitis is diagnosed by a doctor who evaluates symptoms, reviews a medical history, and performs a physical examination. Below are some methods used to diagnose the condition:
- Medical history and symptom assessment: The doctor begins by listening to the patient's symptoms and medical history. Details such as the duration of symptoms, their severity, location, and other accompanying symptoms are important. This information can help narrow down the possible causes.
- Physical exam : Your doctor will assess your lymph nodes for swollen, tender, red, and other symptoms. They may also examine other physical findings to look for clues about the extent of the infection or other underlying conditions.
- Blood tests: Blood tests can indicate the presence of infection or inflammation. Your doctor may order tests such as a complete blood count (CBC) and CRP (C-reactive protein).
- Imaging tests: If necessary, imaging tests may be performed to confirm a diagnosis of adenitis or to rule out other causes. These may include ultrasounds or computed tomography (CT) scans.
- Biopsy : In rare cases, a sample of the lymph node may need to be taken to confirm the diagnosis. The biopsy is sent to a laboratory to examine the cells in the lymph node.
The disease is diagnosed by combining symptoms, physical examination findings, and diagnostic test results. Diagnosis aims to identify the underlying cause and develop an appropriate treatment plan. Therefore, it is recommended that individuals experiencing symptoms consult a doctor.
How is Adenitis Treated?
Treatment for adenitis aims to control the infection and relieve symptoms by targeting the underlying cause. The treatment plan may vary depending on the type of disease, the severity of the infection, the patient's overall health, and other factors. Common treatment methods include:
- Antibiotic treatment: In cases of bacterial adenitis, doctors usually prescribe appropriate antibiotics. These antibiotics help control the infection and prevent the spread of bacteria. The duration of treatment and the antibiotic used depend on the type of infection and the patient's condition.
- Antiviral treatment: In the case of viral adenitis, antiviral medications are generally not used. Viral infections usually resolve on their own. Supportive treatments such as rest, increased fluid intake, and pain relievers or antipyretics can be used to relieve symptoms.
- Managing pain and fever: Pain, tenderness, and fever often occur with adenoiditis. Pain relievers (such as paracetamol or ibuprofen) or antipyretics may help relieve symptoms. However, it's important to consult your doctor before using medication.
- Relieving symptoms: Home measures such as rest, increasing fluid intake, and using a moisturizing mouthwash or nasal spray may help relieve symptoms.
- Treating the underlying condition: Adenitis can sometimes be a symptom of an underlying infection or other health problem. In this case, treatment for adenitis involves treating the underlying condition. For example, dental treatment may be necessary for adenitis caused by a tooth infection.
Treatment for adenitis usually results in improvement of symptoms. However, if your symptoms worsen or persist for an extended period, it's important to seek medical attention. Your doctor will monitor your treatment and may order additional tests or procedures if necessary.
What are the risk factors for adenitis?
- Age: The disease is more common in children and teenagers. Because their immune systems are not yet fully developed, they are more vulnerable to infection.
- Weak immune system: People with weakened immune systems may be at increased risk of developing the disease. Conditions that can weaken the immune system include immune disorders, immunosuppressive treatments, HIV/ AIDS , autoimmune diseases, or taking immunosuppressive medications after an organ transplant.
- Frequent infections: Frequent exposure to recurring infections can increase the risk of illness. Recurrent throat or skin infections, in particular, can lead to bacterial infections that can lead to adenitis.
- Inadequate hygiene: Failure to follow hygiene rules can increase the risk of infection. Touching the mouth or nose with unclean hands or being in contaminated environments can increase the risk of illness.
- Trauma or surgery: Trauma or surgery to the neck or lymph node area can increase the risk of adenitis. For example, infection following a tooth extraction or the disease may develop after neck trauma.
- Smoking: Smoking can weaken the immune system and increase the risk of infection, which can increase the risk of adenitis.
- Personal or family history: People who have had the disease before or have a family history of adenitis may be at increased risk.
While adenitis risk factors increase a person's likelihood of developing the disease, having any risk factor doesn't necessarily mean they will get the disease. These are simply factors that increase the potential risk.
What Complications Does Untreated Adenitis Cause?
- Spread of inflammation : The disease is usually caused by infection. If left untreated, the infection can spread beyond the lymph nodes. In this case, the infection can spread to surrounding tissues and organs, leading to serious complications such as septicemia (blood infection) or abscess formation.
- Abscess formation: In untreated cases, the infection can cause an abscess (a collection of pus) to form in a lymph node. An abscess is often characterized by swelling, pain, and tenderness and may require surgery.
- Chronic adenitis: Untreated or recurring adenitis can become chronic. The disease can lead to recurring infections that cause persistently swollen lymph nodes and symptoms (pain, tenderness, swelling).
- Spreading infections: If the condition is left untreated, the infection can spread to other areas. For example, cervical adenitis can cause the infection to spread to other lymph nodes in the neck or to nearby tissues.
- Progression of underlying infection: The condition may be a symptom of an underlying infection. If left untreated, the underlying infection can progress and damage adjacent organs or systems. For example, if adenitis due to a dental infection is left untreated, the infection can spread to surrounding tissues and cause serious complications such as a tooth abscess, bone infection, or sinus infection.

